ICU Ventilator Strategy
Permissive Hypercapnia Explained: ARDS, PaCO₂, pH, and Ventilator Strategy
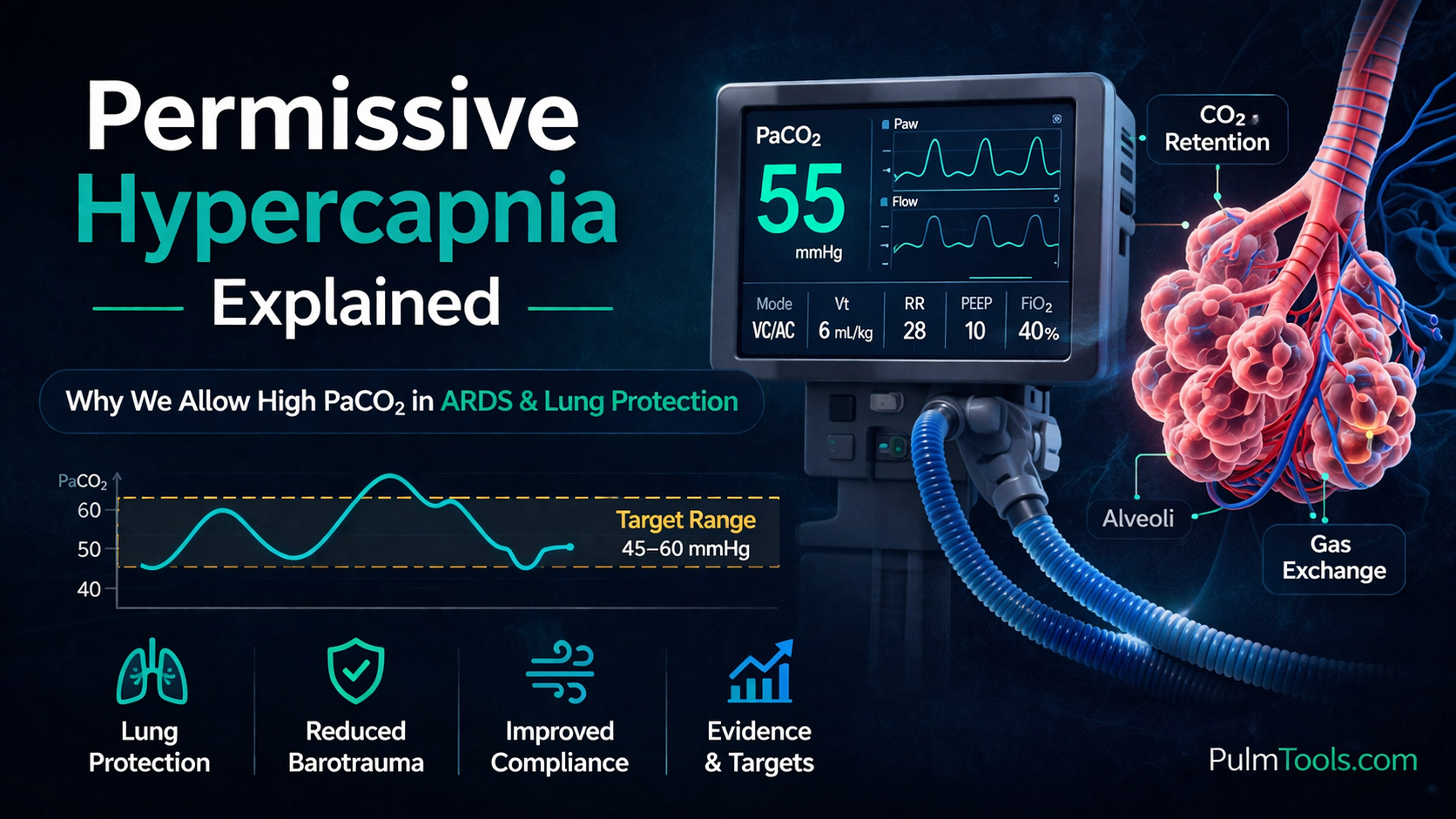
Permissive hypercapnia means intentionally allowing a higher PaCO₂ than normal when trying to force CO₂ down would require unsafe ventilator settings. This beginner-friendly guide explains the concept, why it matters in ARDS and obstructive lung disease, and how clinicians balance lung protection against pH tolerance.
If you need a deeper ICU workflow after this overview, read the Permissive Hypercapnia ICU Guide. For bedside tools, pair this page with our ARDSnet Assistant, ARDSNet Protocol Explained guide, PEEP/FiO₂ table guide, and the Desired PaCO₂ / VE calculator. For blood gas interpretation during ventilator changes, also review our ABG Interpretation guide, ABG Analyzer, and P/F Ratio guide.
What Is Permissive Hypercapnia?
Permissive hypercapnia means intentionally tolerating an elevated PaCO₂ to avoid causing more harm with the ventilator. Instead of pushing the respiratory rate, tidal volume, or pressure high enough to force a normal CO₂, clinicians accept a higher CO₂ level in order to preserve lung-protective ventilation.
In practice, this usually comes up in ARDS, severe obstructive lung disease, and other situations where aggressive ventilation could worsen barotrauma, volutrauma, auto-PEEP, or dynamic hyperinflation.
Quick Definition
In plain language, permissive hypercapnia means: “We are accepting a higher CO₂ because the safer ventilator strategy matters more than forcing a normal CO₂ right now.” The strategy is intentional, monitored, and usually tied to lung protection.
Why Clinicians Use Permissive Hypercapnia
The core idea is simple: sometimes normalizing PaCO₂ is not worth the price. If the patient would need unsafe tidal volumes, higher plateau pressures, or excessively aggressive settings to achieve a normal CO₂, the ventilator may create more injury than benefit.
- Protects against ventilator-induced lung injury
- Supports low tidal volume ventilation in ARDS
- Helps avoid excessive airway pressures
- May reduce overdistension when lung compliance is poor
This is why permissive hypercapnia is tightly linked to the ARDSNet protocol and the broader concept of lung-protective ventilation.
When It Is Commonly Used
ARDS
This is the classic setting. Clinicians often accept higher PaCO₂ to maintain low tidal volume ventilation and safe plateau pressures.
Severe Obstructive Disease
In asthma or COPD with air trapping, avoiding aggressive minute ventilation can be safer than forcing a normal CO₂ and worsening dynamic hyperinflation.
If the patient has ARDS, use this page together with the ARDSnet Assistant and our Causes of Hypoxemia guide to frame the bigger oxygenation picture.
Bedside Ventilator Strategy
Permissive hypercapnia is not “do nothing.” It is an intentional trade-off made after prioritizing lung safety. In ARDS, clinicians usually think in this order:
- Set a lung-protective tidal volume strategy
- Watch plateau pressure and driving pressure
- Use appropriate PEEP/FiO₂ strategy
- Accept a higher PaCO₂ when normalizing it would require unsafe ventilation
When you need help estimating how minute ventilation changes may affect PaCO₂, the Desired VE calculator is one of the most useful bedside tools on PulmTools. It works especially well when used together with the PaCO₂ calculator, the ARDSNet calculator, and the PEEP/FiO₂ table guide.
PaCO₂, pH, and Practical Targets
In real practice, clinicians do not usually chase a single “magic PaCO₂.” The more useful question is whether the patient is tolerating the resulting pH, hemodynamics, and overall strategy.
- Higher PaCO₂ may be acceptable if pH remains tolerable
- Trend the patient, not just the blood gas number
- Reassess mental status, hemodynamics, and work of breathing
- Use ABGs to make sure the strategy is behaving as expected
For blood gas pattern recognition, use our ABG Interpretation guide and ABG Analyzer.
Risks, Cautions, and When to Be Careful
Permissive hypercapnia is useful, but it is not harmless. A rising CO₂ can affect pH, cerebral blood flow, hemodynamics, and the patient’s overall clinical trajectory.
- Severe acidemia may not be tolerated
- Intracranial pathology may limit tolerance for high CO₂
- Hemodynamic instability changes the risk-benefit balance
- Progressive deterioration may mean the strategy is failing, not succeeding
This is why permissive hypercapnia should always be framed as a clinical strategy, not just a lab abnormality.
Related Guides
FAQ
What is permissive hypercapnia?
Permissive hypercapnia is the intentional acceptance of a higher PaCO₂ to preserve lung-protective ventilation and avoid injurious ventilator settings.
Is permissive hypercapnia the same as respiratory acidosis?
Not exactly. Permissive hypercapnia often causes or accepts respiratory acidosis, but the term refers to the deliberate ventilator strategy of tolerating elevated PaCO₂ for lung protection.
Why is permissive hypercapnia used in ARDS?
In ARDS, normalizing CO₂ may require tidal volumes or pressures that increase lung injury. Permissive hypercapnia supports the lung-protective ARDSNet strategy.
Does permissive hypercapnia mean ignore the ABG?
No. You still trend ABGs, pH, hemodynamics, and overall clinical response. The point is to interpret the blood gas in the context of lung protection, not to chase a normal number at all costs.
Bottom Line
Permissive hypercapnia is not a mistake — it is often a deliberate ICU decision. In ARDS and other high-risk ventilator situations, accepting a higher PaCO₂ can be the safer path when the alternative is more lung injury. The key is to balance lung protection, pH tolerance, and the patient’s overall trajectory.