Respiratory Failure Basics
Oxygenation vs Ventilation: ABG Clues, PaO₂, PaCO₂, and Bedside Strategy
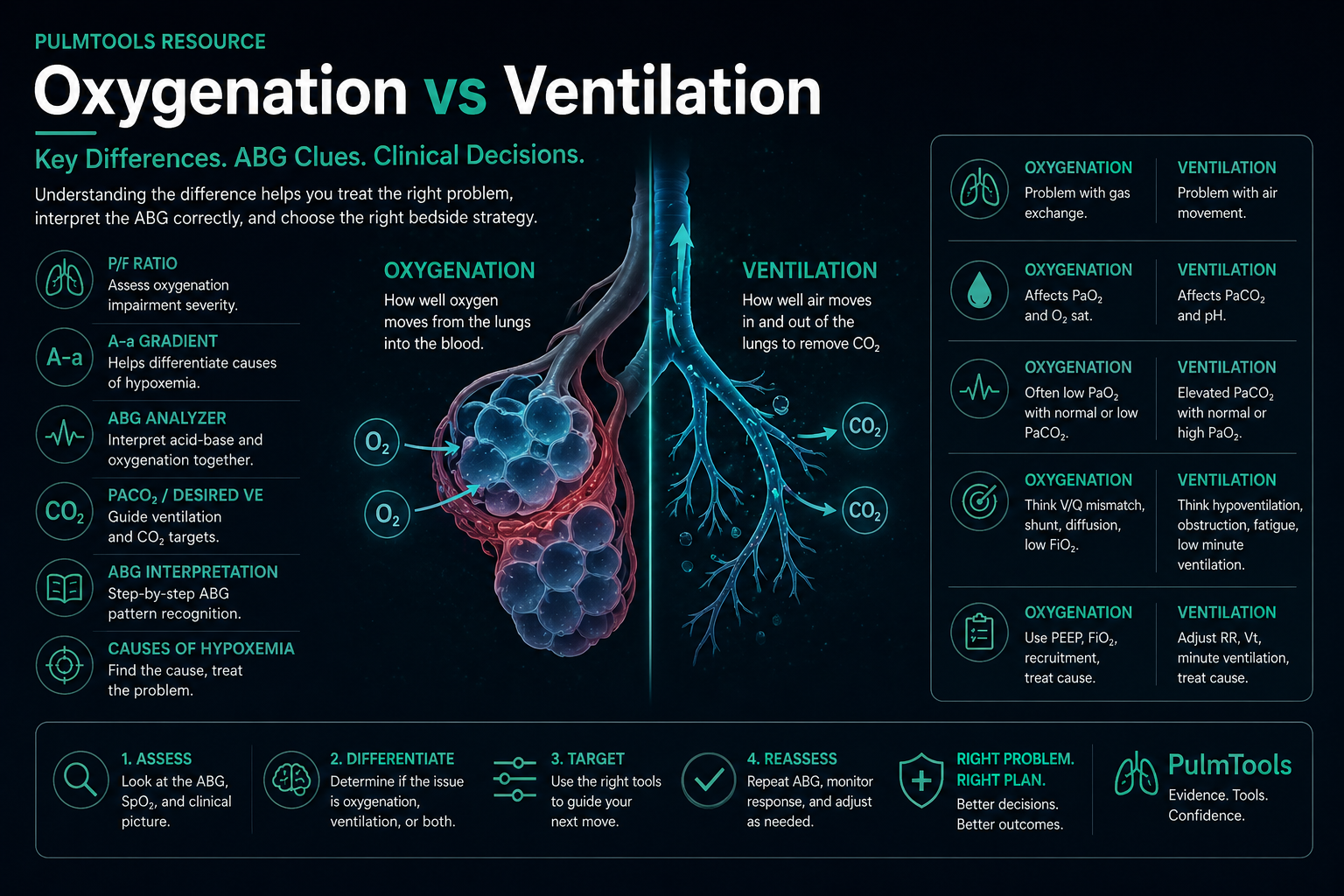
Oxygenation and ventilation are related, but they are not the same problem. Oxygenation is about getting oxygen into the blood. Ventilation is about moving air in and out of the lungs to remove CO₂. Understanding the difference helps you interpret ABGs correctly, choose the right respiratory support, and avoid treating the wrong problem.
Use this guide with the ABG Analyzer, P/F Ratio Calculator, A–a Gradient Calculator, PaCO₂ Calculator, and Desired VE Calculator when you need to connect ABG interpretation to bedside respiratory decisions.
Quick Answer
Oxygenation asks, “Is enough oxygen getting into the arterial blood?” It is mainly reflected by SpO₂, PaO₂, P/F ratio, and sometimes A–a gradient. Ventilation asks, “Is enough CO₂ being removed?” It is mainly reflected by PaCO₂, pH, minute ventilation, respiratory rate, tidal volume, and work of breathing.
Oxygenation vs Ventilation at a Glance
| Question | Oxygenation | Ventilation |
|---|---|---|
| Core problem | Gas exchange and oxygen transfer into arterial blood | Air movement and CO₂ removal from the lungs |
| Main ABG clue | Low PaO₂ or low oxygen saturation | High or low PaCO₂ with pH change |
| Useful tools | P/F ratio, A–a gradient, oxygenation index, SpO₂ trend | PaCO₂ trend, desired VE, minute ventilation, ABG interpretation |
| Common causes | V/Q mismatch, shunt, diffusion impairment, low FiO₂, atelectasis | Hypoventilation, obstruction, fatigue, oversedation, neuromuscular weakness |
| Common interventions | Increase FiO₂, optimize PEEP, recruit lung, treat the cause | Adjust respiratory rate, tidal volume, pressure support, minute ventilation, or ventilatory support |
ABG Clues: PaO₂ vs PaCO₂
On an ABG, PaO₂ helps you understand oxygenation, while PaCO₂ helps you understand ventilation. A patient can have an oxygenation problem without a ventilation problem, a ventilation problem without severe hypoxemia, or both at the same time.
- Low PaO₂ with normal or low PaCO₂: think oxygenation failure, such as V/Q mismatch, shunt, diffusion impairment, or low FiO₂.
- High PaCO₂ with acidemia: think ventilatory failure or hypoventilation.
- Low PaCO₂ with alkalemia: think hyperventilation or respiratory alkalosis.
- Low PaO₂ plus high PaCO₂: both oxygenation and ventilation may be failing.
For a step-by-step acid-base workflow, use the Step-by-Step ABG Interpretation guide and the ABG Practice Examples.
When the Problem Is Oxygenation
Oxygenation problems usually show up as low SpO₂, low PaO₂, increasing oxygen requirement, or worsening P/F ratio. The next step is to decide whether the problem is severity, mechanism, or response to support.
Quantify severity
Use the P/F Ratio Calculator to compare PaO₂ to FiO₂ and track hypoxemic respiratory failure.
Think through the cause
Use the A–a Gradient Calculator and the Causes of Hypoxemia guide to separate V/Q mismatch, shunt, diffusion impairment, and hypoventilation patterns.
When the Problem Is Ventilation
Ventilation problems usually show up as PaCO₂ moving in the wrong direction, pH changing with CO₂, rising work of breathing, or inadequate minute ventilation. In ventilated patients, the question becomes whether the current minute ventilation matches the desired CO₂ goal safely.
Estimate CO₂ response
Use the Desired VE Calculator and PaCO₂ Calculator to connect minute ventilation changes with PaCO₂ targets.
Protect the lung
In ARDS or severe lung disease, use the ARDSNet Calculator and review Permissive Hypercapnia Explained before chasing a normal CO₂ with unsafe settings.
Bedside Strategy: Treat the Right Problem
- Look at the ABG, SpO₂, FiO₂, respiratory rate, work of breathing, and clinical trajectory together.
- Decide whether the dominant issue is oxygenation, ventilation, or both.
- For oxygenation failure, think FiO₂, PEEP, recruitment, shunt, V/Q mismatch, and underlying cause.
- For ventilation failure, think minute ventilation, airway resistance, fatigue, obstruction, sedation, and ventilatory support.
- Reassess after any intervention with vitals, work of breathing, pulse oximetry, and repeat blood gas when clinically needed.
Related PulmTools Resources
FAQ
What is the difference between oxygenation and ventilation?
Oxygenation is the process of getting oxygen into arterial blood. Ventilation is the process of moving air in and out of the lungs to remove carbon dioxide.
Which ABG value reflects oxygenation?
PaO₂ is the main ABG value used to assess arterial oxygenation. SpO₂, FiO₂, P/F ratio, and A–a gradient can add important context.
Which ABG value reflects ventilation?
PaCO₂ is the main ABG value used to assess ventilation. High PaCO₂ suggests hypoventilation or ventilatory failure, while low PaCO₂ suggests hyperventilation.
Can a patient have both oxygenation and ventilation failure?
Yes. A patient can have low PaO₂ and high PaCO₂ at the same time, especially in severe respiratory failure, fatigue, obstructive disease, or advanced parenchymal lung disease.
Bottom Line
Oxygenation and ventilation answer different bedside questions. If PaO₂ or SpO₂ is the problem, think oxygen transfer and gas exchange. If PaCO₂ and pH are the problem, think ventilation and CO₂ removal. The best respiratory plan starts by identifying which problem you are actually treating.